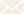How do you live a normal life when you have trouble breathing? This blog will introduce you to the different respiratory conditions and show you how treatments and daily living products will help you cope with respiratory diseases.
What is a respiratory disease?
A respiratory condition is an illness that affects your respiratory system or the organs related to breathing and respiration. This includes the airways, the lungs, and the chest.
There are many diseases that affect the lungs. These include COPD, Asthma, Emphysema, Acute lower respiratory tract infections and Cystic Fibrosis. Illnesses related to respiratory diseases affect almost a third of Australians and are a costly endeavour for the Australian healthcare system.
So how do you live a normal life when you have trouble breathing? This blog will introduce you to the different respiratory illnesses and show you how treatments and daily living aids can help you adapt to live a normal life.
Two categories of lung diseases
There are two categories into which respiratory conditions can be divided.
Respiratory infection: viral or bacterial
These are usually short term or acute lung diseases, if they are addressed, treated (and if the body responds well to treatment), and well managed. The respiratory infection diseases include the flu (influenza) and respiratory viruses such as currently Covid-19.
Antibiotics are not effective for viral infections which leaves the condition to run its course for the most part. Bedrest and keeping warm is the best way to speed up the recovery. In the case of a bacterial infection, antibiotics can be administered to help treat the infection.
Chronic lung diseases
Chronic lung diseases are respiratory conditions that affect the airways, like asthma, emphysema, Cystic Fibrosis and COPD. These diseases are not curable.
The two most common chronic lung conditions are asthma and COPD. It can be difficult to differentiate COPD from asthma because the symptoms of both conditions can be similar, although some important features distinguish COPD from asthma. The most important one is that people with COPD continue to lose lung function despite taking medication, whilst that is not the case with asthma.
With chronic lung diseases, antibiotics are used to treat existing infections to reduce the risk of infections in the future.

How do you manage a respiratory disease?
There are so many challenges you face if you have a chronic respiratory disease. If you need oxygen, you probably feel self-conscious to go out in public. You might become very aware of your chronic cough and feel embarrassed when you are around people. These feelings are tough to try and process.
You might also be finding it difficult to let go of the activities you have always enjoyed in your life. You might no longer be able to travel as easily, participate in dancing, work in the garden, walk or exercise and spend time with family as easily as you did before.
Adequate lung care is important but taking these changes into your stride isn’t easy, so don’t feel as though you have to simply accept it. Leaving these activities behind can be akin to grieving the loss of a loved one because you are essentially letting go of the life you have always had. Understand that this new lifestyle is something to grasp and accept over a period of time. Be patient with yourself; learn more about your disease and how to make lifestyle adjustments to improve your quality of life.
Asthma

Asthma is a common debilitating chronic disorder of the lungs that can be life-threatening. Asthma in Australia is amongst the highest in the world: 1 in 9 people or 2.7 million Australians had asthma in 2020-21 with up to 16% of children and around 12% of adults affected.
What causes asthma?
Asthma is characterised by the narrowing of the airways in response to a trigger. Most people can tolerate breathing in dust or pollen, but someone who suffers from asthma will have difficulty breathing when they come into contact with pollutants or impurities in the air. When triggered, an asthmatic person suffers an asthma attack - their airways narrow because the muscles tense and the lining of the airway becomes inflamed and coated with mucus. Triggers can include exercise, common colds, airborne pollutants like smoke, and impurities in the air or allergens like dust, dust mites, and pollen.
What are asthma signs?
Asthma is an immune lung disease of which the symptoms differ per person. Some asthma sufferers may have all the symptoms while others only have one or two. The most common symptoms of asthma are:
- Tight chest
- Shortness of breath
- Wheezing, or a whistling sound made when breathing
- Dry, persistent cough: mostly during exercise, at night or early morning
- Fatigue
It can be very scary to see someone having moderate to severe asthma symptoms. What do you do? Do you treat him/her at home, make an urgent appointment with your GP or asthma nurse or call an ambulance? Knowing the signs of an asthma attack and taking action can save their life. The symptoms of an asthma attack are: struggling to breathe, tight chest and wheeze.
What are asthma treatments?
Unfortunately, there is no cure for asthma. The condition can only be managed by staying aware of triggers and minimising them from the environment, and by keeping medicines at hand. Adequate lung care is also important. In consultation with an asthma specialist, a personalised asthma management plan will be developed and put in place for the patient.
Breathing tests are essential to check if your asthma is not under control. A peak flow meter measures how fast you can force air out of your lungs. A spirometer is a breathing exerciser to measure your inhalation and improve your lung fitness.
There are a number of treatment options available for asthma. These treatments can stop an asthma attack, preventing it from becoming life-threatening. Therapy options include;
- Relievers: these help to open up airways during an asthma attack to enable easier breathing
- Preventers: these anti-inflammatory steroids help to prevent asthma attacks when taken daily
- Combination preventers: this medicine contains two active components - a long-acting airway relaxer and an anti-inflammatory steroid preventer.
Spacers and nebulisers – either with a mouthpiece or a mask - can be used with both inhalers. Spacers are holding chambers that make it easier to take the medication from a metered dose inhaler, or MDI. Spacers are available in a disposable or reusable form.

Nebulisers are reliable breathing treatment machines that turn the liquid medication into a fine mist that can reach the lungs directly. Make sure you know how to use your asthma medication properly.
COPD

COPD is a blanket term for a group of lung diseases that affect the lungs and progressive. Australia saw 1 in 20 Australians over the age of 45 with COPD (chronic obstructive pulmonary disease) in 2018.
The most common examples of COPD include emphysema and chronic bronchitis. Many people suffer from both simultaneously. COPD is most commonly caused by long-term exposure to irritants in the air and cigarette smoke inhalation. Unlike an infection, it is developed over time.
What are the symptoms of COPD?
The early stage of COPD presents with symptoms like;
- occasional shortness of breath, especially after exercise
- mild but recurrent cough
- needing to clear your throat often, especially first thing in the morning
The symptoms typically progress to;
- wheezing
- shortness of breath
- chest tightness
- chronic cough
- need to clear mucus from your lungs every day
- frequent colds, flu, or other respiratory infections
- lack of energy
- fatigue
- swelling of the feet, ankles, or legs
- weight loss
What are the treatments of COPD?
There is no cure for COPD, it is a group of conditions that all gradually progress. There are ways to make living with COPD easier. There are treatments that reduce the intensity of symptoms to make life a little easier. Adequate lung care is vital.
The most common medical treatments to ease the symptoms of COPD include
- bronchodilators - to relax the muscles in the airways and allow more air through
- corticosteroids - to relax airways for better airflow
- PDE-4 inhibitors or Phosphodiesterase-4 inhibitors - reduce inflammation, especially useful for those with chronic bronchitis
Inhalers or puffers are used to get the medication to the lungs. If you have difficulty using an inhaler, your doctor will recommend you use a nebuliser. A nebuliser turns liquid medication into a fine mist which is inhaled via a mask or a mouthpiece into your lungs.

A spacer is an attachment that fits onto the puffer or inhaler and helps get your medication to your lungs without waste or without it ending up inside your mouth (instead of your lungs). You might find it helpful to use the device if you have problems timing inhalation with the spray. They are especially useful for children. Spacers are available in disposable or re-usable models.
Emphysema

Emphysema is a progressive lung disease, and one of the primary diseases under the category of COPD. Most cases of emphysema happen as a result of tobacco use over a period of years. Non-smokers can also get emphysema, but smokers are far more likely to suffer from this condition. The smoke damages the fragile air sac linings of the lungs. As a result, the lung takes on tiny pockets of air and the lungs start to enlarge. This can make it difficult to breathe. Over time, more and more air gets trapped between the damaged tissues in the lungs.
Emphysema is diagnosed by testing the function of the lungs. Testing for emphysema means assessing airflow limitations. If you battle to expel air from your lungs as fast as you should, this could be a sign of emphysema. Doctors recommend that smokers who are diagnosed with emphysema kick the habit as soon as possible. This sadly won’t reverse the damage, but it will prevent more damage or at least slow the progression of the illness.
It’s not only smokers that get emphysema. There is another rare condition that often results in the body’s own white blood cells damaging the lungs which eventually leads to emphysema. An AAT deficiency means the body isn’t producing enough of the natural protein that is responsible for preventing white blood cells from attacking the body. This means that the presence of white blood cells will naturally cause damage to your lungs. For a smoker, this condition is far more severe.
What are the symptoms of emphysema?
The symptoms of emphysema include;
- Shortness of breath quickly (your muscles have to work harder to help you breathe)
- Wheezing
- A cough that won’t go away
- Chest tightness or pain
- Loss of appetite
- Sleep problems
- Blue lips or nail beds
- Fatigue
- Frequent lung infections
- Morning headaches
- Weight loss
- Depression
- Problems having sex
Can emphysema be treated?
Emphysema, like other forms of COPD and asthma, can’t be cured but the symptoms and the progression of the disease can be managed. This can help you to feel more comfortable and empowered. Adequate lung care is vital.
Treatment protocols for emphysema include;
- bronchodilators - to relax the muscles in the airways and allow more air through
- corticosteroids - to relax airways for better airflow
- PDE-4 inhibitors – the newer medication Phosphodiesterase-4 inhibitors reduce inflammation and improves lung function
- oxygen therapy – will supplement oxygen to help you breathe on your own
Inhalers or puffers are used to get the medication to the lungs. A nebuliser is a handy machine that delivers medication via a mask or mouthpiece. They are often recommended for those patients who have trouble using an inhaler or cannot inhale deeply enough for other devices.
An estimated 90% of lung patients use their inhaler incorrectly meaning a waste of medication and a lower deposition of the medication in the lungs. That is when a spacer comes in handy. A spacer is a holding chamber that attaches to the inhaler and is an effective solution to help with the delivery of the medication straight to the lungs. It should always be used with corticosteroids. They are available in disposable or re-usable models. They are very suitable, if you find it difficult timing the spray with inhalation.

GP’s will recommend you get a yearly flu vaccine and the pneumonia shot every 5 to 7 years to prevent serious lung problems.
For more details on emphysema, we recommend visiting the website of Lung Foundation Australia.
Acute lower respiratory tract infections
A lower respiratory tract infection is categorised by location - any infection that relates to the respiratory system and takes place under the voice box, is a lower respiratory tract infection. Examples of these conditions include tuberculosis (TB), pneumonia, bronchitis.
Symptoms of an acute lower respiratory tract infection
It can be difficult to tell if you have a lower respiratory tract infection because in the early stages, the symptoms are very similar to a severe cold or flu. A severe infection might give you great discomfort and make itself obvious early. A mild infection can be less obvious.
Mild symptoms might present with:
- a stuffed up or a runny nose and a dry cough
- fever
- sore throat
- headache
Severe infections might present with symptoms such as:
- a severe/phlegmy cough
- fever
- difficulty breathing
- a blue tint to the skin
- rapid breathing
- chest pain
- wheezing
What causes a lower respiratory tract infection?
There are a number of possible causes for contracting a lower respiratory tract infection. It can be as a result of a viral infection, like influenza or RSV. Fungal infections, too, can lead to infections that affect the lower respiratory tract. A bacterial infection caused by Streptococcus or Staphylococcus aureus is also a common cause for acute lower respiratory tract infections.
Environmental triggers for these illnesses include:
- tobacco smoke
- dust
- chemicals
- vapours and fumes
- allergens
- air pollution
You are more likely to suffer from an acute lower respiratory tract infection if you have recently had a cold or the flu. Those with a compromised immune system, like diabetics, are more likely to contract an infection, as are those who are older than 65 years and those who are younger than 5 years.
Lung care is essential, this includes staying away from smoke and pollutants.
Is there a treatment for a lower respiratory tract infection?
There is not a great deal of treatment options for these acute viral infections. You can get some over the counter medications to boost your immune system and reduce the symptoms but the best way to combat the illness is with bed rest.
The treatment of Bronchitis or pneumonia depends if it is bacterial or viral. If the cause is bacterial, patients will be treated with antibiotics. For severe cases, your GP might also prescribe oxygen therapy to help you breathe more comfortably.
Cystic Fibrosis

Cystic fibrosis (or CF) is a condition that is genetic, meaning you are born with this respiratory disease as it is inherited from both parents. In Australia, 1 in 2,500 babies are born with CF. 1 in 25 people carry the CF gene, but most are not aware they are carriers as they show no symptoms and live normal lives. That means about 1 million Australians are unaware carriers.
Cystic Fibrosis Australia explains it perfectly: “Cystic Fibrosis primarily affects the lungs and digestive system because of a malfunction in the exocrine system that’s responsible for producing saliva, sweat, tears and mucus”. In healthy people these secretions act as a lubricant and are normally thin and slippery. In people with CF a defective gene causes it to become thick and sticky.
Cystic Fibrosis is a progressive disease; it tends to worsen over time making breathing more and difficult because it brings about frequent lung infections.
Symptoms of Cystic Fibrosis
The symptoms of cystic fibrosis vary per person and can develop soon after birth, start in early childhood or may not be obvious until adulthood. The main symptoms of CF often include:
● Salty skin
● Recurring lung infection, pneumonia, and bronchitis
● Lingering cough, with or without phlegm
● Wheezing
● Shortness of breath
● Poor weight gain
● Fatty bowel movements or diarrhoea
● Male infertility
Those who have the condition can also develop related conditions such as:
- Diabetes
- Thin, weakened bones or osteoporosis
- Liver problems
Treatment for Cystic Fibrosis
Currently there is no cure for CF. Treatment and management of cystic fibrosis is an ongoing, lifelong process. Someone with CF may need up to 4 hours of airway therapy a day. Treatment are available to help control the symptoms, prevent any complication, and make it easier to live with. They generally involve:
- Intensive mucus clearing therapy in the form of physiotherapy to improve breathing techniques and the use of an airway clearance device.
- Special medication to make the mucus thinner and easier to cough up
- Antibiotics to treat and prevent lung infections
- Steroid medication to treat small growths inside the nose
- Bronchodilators to relax and widen the airways: aerosol mist inhalations via a MDI, a nebuliser or soft mist inhaler
- Medicine to help absorb food
- Special diet and supplement to prevent malnutrition
For people with CF it is also important to have a flu shot every year.
Social distancing and infection control are an integral part of the daily life and have been the norm within the routine of CF sufferers in order to keep them safe. Contact with germs and contaminants must be minimised to reduce the risk of infection. For anyone living with cystic fibrosis, medications are an absolute necessity and adequate lung care is vitally important.
For more information on cystic fibrosis, please visit Cystic Fibrosis Australia.
Conclusion
Living with any form of respiratory disease can impact your quality of life. As a result, it can be painfully limiting. You will need medicines to form part of your daily life to simply feel able to function.
It is important to treat your condition as an inevitable part of your life: one that can be managed but one that is never going away completely.
To deal with a lung illness you need to protect yourself first. Exercise, medication and certain daily living aids can help you form a protective health barrier. You cannot cure a respiratory disease but you can cope with the situation by taking care of yourself.
Want to read more on this subject? Here is another blog post you might find interesting:
Enhance your understanding and find practical solutions with our other top-performing blogs:
- A Bottom Wiper: How Can It Help a Bariatric User?
- Find the Best Crutches to Suit Your Needs
- Choosing the Right Walking Frame for Parkinson’s Disease
- What Is Normal Blood Pressure?
- The Benefits of the Multifunctional Chair After Hip or Knee Surgery
- Bathroom Tasks Made Easy for Those Living with Parkinson’s
Stay informed with tips and insights tailored to your needs!
About Bettercaremarket
Bettercaremarket is your leading supplier of healthcare essentials and your #1 destination for quality incontinence supplies, mobility equipment, independent living aids for seniors, disability aids, rehab and therapy products and medical supplies.
We help NDIS-participants, aged care facilities, home care package providers, occupational therapists and allied health providers find the best solutions to solve their need.